Blue Water Cruising Health - How to prepare?
"One boat in every two setting out long-distance has had to deal with a medical problem at sea or at a stopover". This statistic comes from a recent survey conducted by Médidistance (a French organization which assists people preparing for traveling out of range of professional medical help). The question of health at sea arises as soon as you have left the dock, and becomes unavoidable when ocean cruising.
In his preparations, the skipper can put his blind faith in Neptune to look after the boat and the health of the crew. But it’s more sensible if he optimizes everything that he can. Once en route, the management of medical problems is indeed complicated by the degree of isolation in which the sailor is located. Access to help can be a long way away, or difficult. The medical knowledge of the crew, the medical equipment and the means of communication present on board facilitate the management of an incident...

What medical problems are encountered?
In contrast with information from offshore races or shorter nautical events such as the ARC rally, the Médidistance survey was intended to provide an overview of medical problems encountered at sea or at stopovers, by sailors cruising long-term (from 6 to more than 24 months). (Table 1)
The details of the health problems encountered constitute a long and varied list.
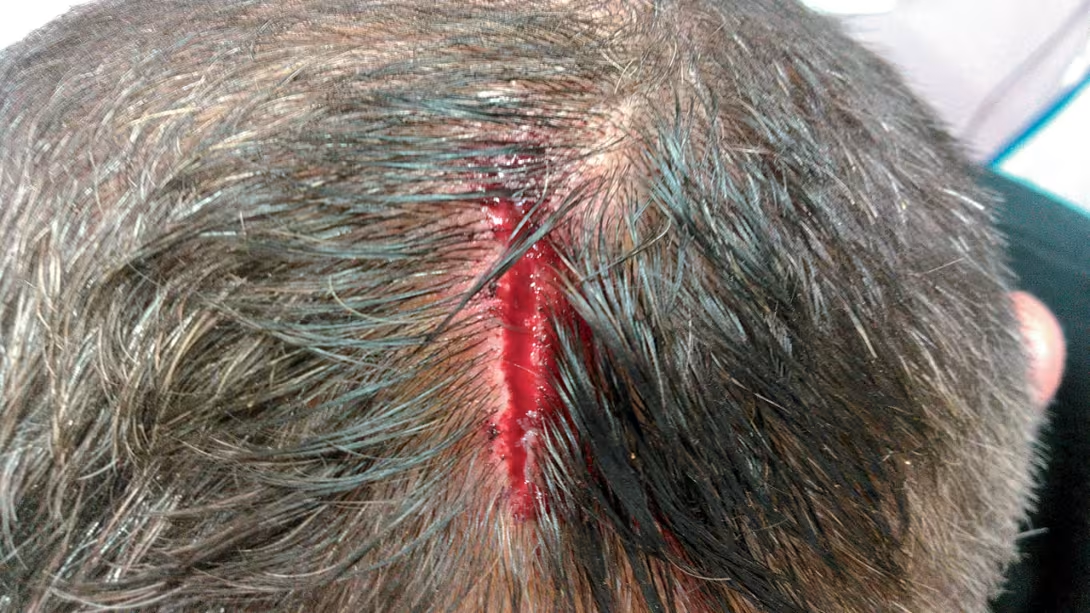
Some crews have been confronted with some serious problems: a head trauma off A Coruña, requiring evacuation, heart attack, deep propeller injury at anchor, kidney stones in the middle of the ocean with no means of communication on board, crush and finger fracture during anchoring maneuvers, infection requiring antibiotic treatment not present on board and the diversion of a freighter during an Atlantic crossing...
Fortunately, other crews had a quieter time of it, but didn’t escape some of the common problems: traveler's diarrhea, ENT or cutaneous disorders, various wounds and fractures...
In general, the survey shows that all the medical problems of our daily life occur at sea or at stopovers and that their gravities are as varied as those encountered in an Emergency Room.
With an equivalent frequency, illnesses and traumas are the cause of problems for the crew (Tables 2 to 4). When cruising, infections are a major cause of illness (50%). Trauma more specific to nautical activities (ropes, winches, fishhooks...) or related to marine wildlife is common.
But the cruising sailor worried by this table can be reassured. Today, it is possible to deal effectively with these medical problems. Specific and adapted medical training is available; the content of the medical kit to be carried aboard is known and validated. And in addition, modern means of communication make it possible to use telemedicine, if necessary.
How to prepare before departure?(3 to 6 months beforehand)
1 - Preparing the crew.
The crew must get in shape for setting off, and check their state of health. The general practitioner should be consulted (advice, checkups, personal treatments and prescriptions, routine vaccinations, etc.) Similarly, a visit to the dentist can avoid problems while cruising. For cruising outside Europe or North America, an appointment at a vaccination and tropical diseases center is recommended (specific or mandatory vaccinations, hygiene advice, and prevention of mosquito-borne diseases)
It is also essential to take out health insurance. There is a wide range of choice: it must be reliable, responsive and adapted. The services of your national Social Security system or help related to credit cards are insufficient or limited in time. The cost of repatriation or care abroad involves amounts that are often much higher than those imagined. For some countries or islands visited, "World coverage” is not sufficient (for example in the US or Puerto Rico or the USVI).
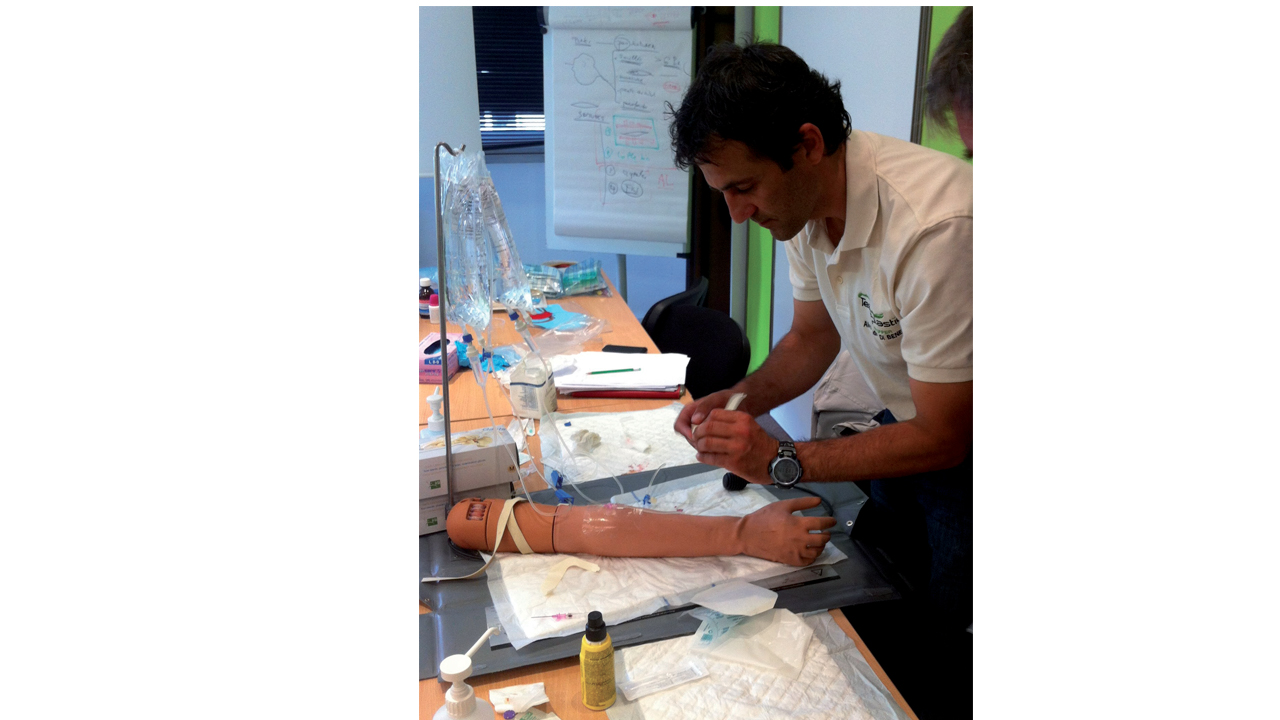
2- Improving the medical skills on board: What training?
The crew can improve their medical skills, acquire appropriate reflexes and learn some essential technical actions. The goal is obviously not to solve every medical problem on board by oneself, but it is useful to be able to assess the need to contact a doctor for advice and, once in contact with him or her, to be able to become their eyes and hands to assess the seriousness of the problem, to make a diagnosis and to instigate the necessary treatment.
Here in France, for sailors or ocean racing competitors, the French Sailing Federation offers two types of training through validated training centers. The first, called "PSMer" - First Aid at Sea, is a short training course. In one day, it provides the basics of the first response to an emergency. It is mainly intended for racers and coastal cruisers. The second called "FMH" (Offshore Medical Training) offers very comprehensive content, studied over three days and intended primarily for competitors in ocean races such as the Vendée Globe. Similarly, in the UK and various other countries, Maritime Academies for the merchant marine offer different courses, including MCA STCW Proficiency in Medical First Aid On Board Ship and MCA STCW Proficiency in Medical Care On Board Ship. An internet search will quickly reveal the kind of training available in North America and elsewhere.

For crews, such as a family or a couples, or single-handers setting off for an Atlantic circuit or a circumnavigation, training better suited to this type of "Blue Water" project also exists.
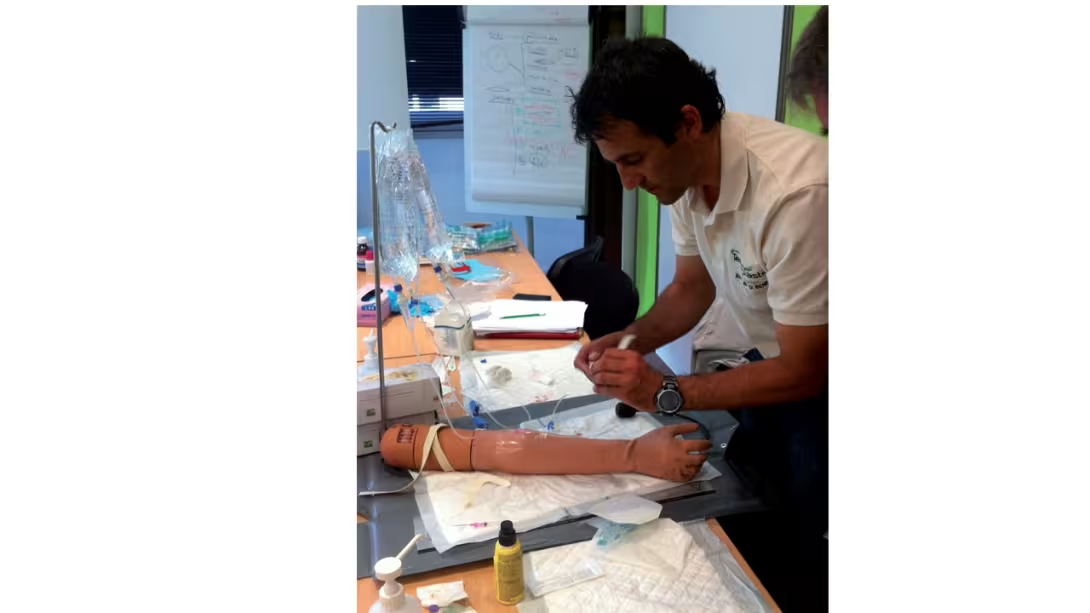
In France, they are offered by different centers around the country (see Table 5) and carried out over two days. Called "Offshore cruising Medical" or "Learning Medical Techniques in Isolated Situations", etc, their content is essentially practical, and within reach of all sailors. Medical jargon is put aside, and practical workshops, situations and genuine case studies follow one another throughout these courses, which are very popular with all who attend.
The topics covered are multiple. Each participant gets a reference diagram that allows him to evaluate a medical problem, and this is the basis of the training. This makes it possible to assess the seriousness of a situation and the need for a medical remedy. The understanding of the organization of medical aid at sea is a prerequisite to contact available consultation facilities or medical assistance correctly and without losing time.
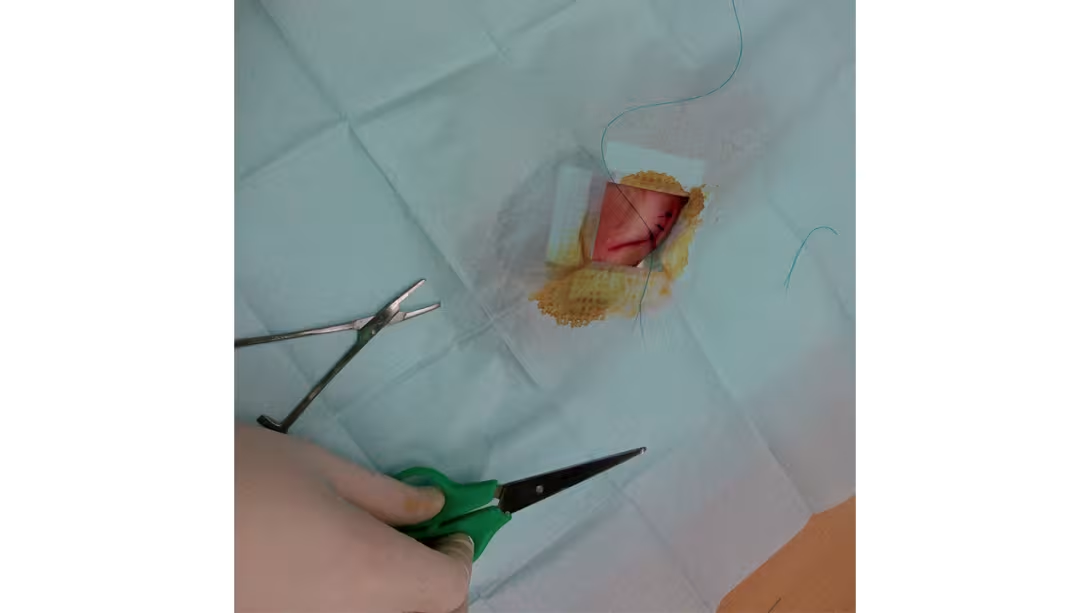
Urgent actions to be performed are learned (fainting, cardiac arrest, drowning, hypothermia, choking...). The warning signs and the severity of medical problems are discussed (abdominal or thoracic pain, dehydration, allergies...). The management of the different types of trauma (burns, hemorrhaging, fractures and sprains) is detailed. Technical actions that the crew may have to carry out are performed (skin sutures, intramuscular injection, etc.) as part of the training.
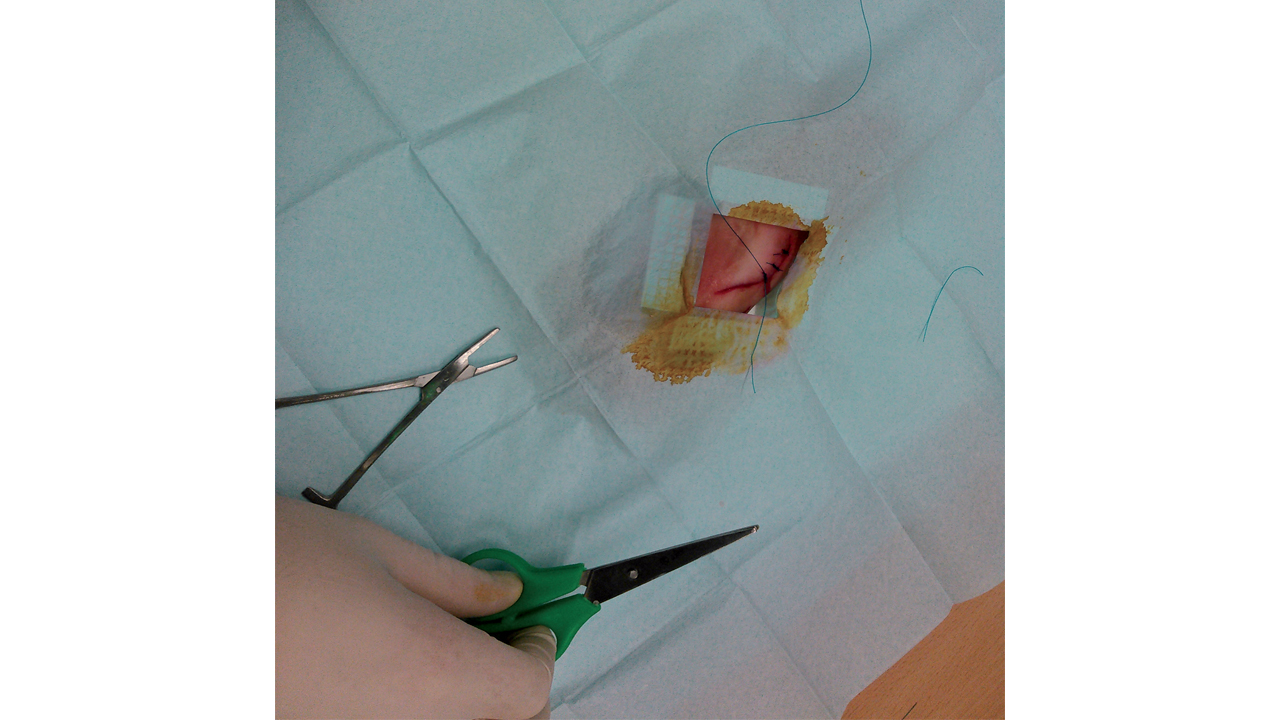
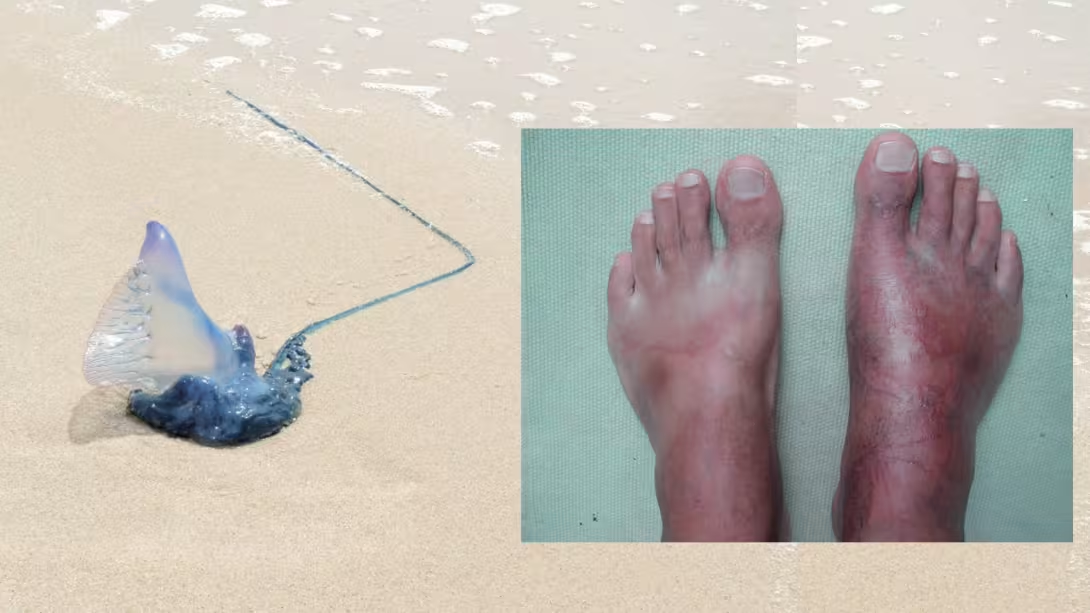
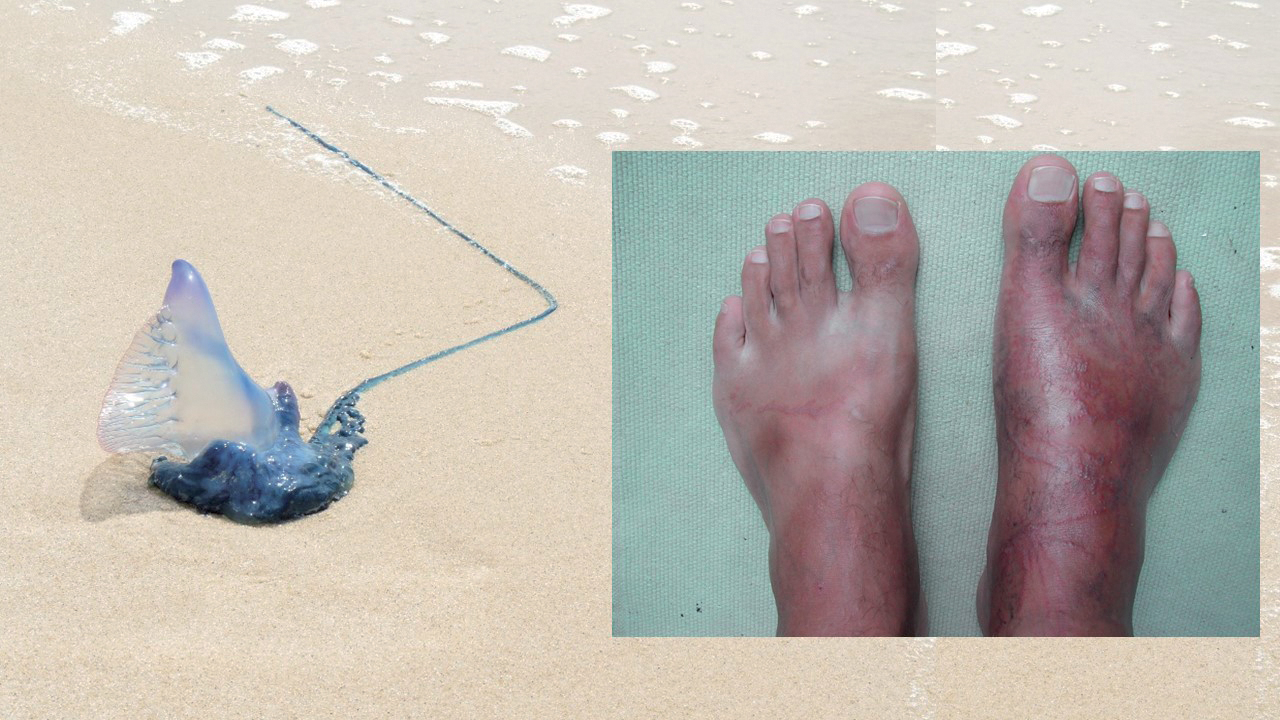
The importance of the prevention of accidents and diseases on board is essential to the participants of any blue water medical training program. Although the turquoise waters will serve as idyllic scenery throughout the trip, wildlife and the marine environment (jellyfish, stone fish, ciguatera...) can stop you in your tracks. It’s important to know about them so you can anticipate and avoid them.
These training courses are also an opportunity to review your on-board medical kit and adapt its contents.
3- How to equip the boat?
In addition to the medical knowledge on board, the ease of management of medical problems encountered is helped greatly by having suitable medical equipment on board, and effective means of communication.
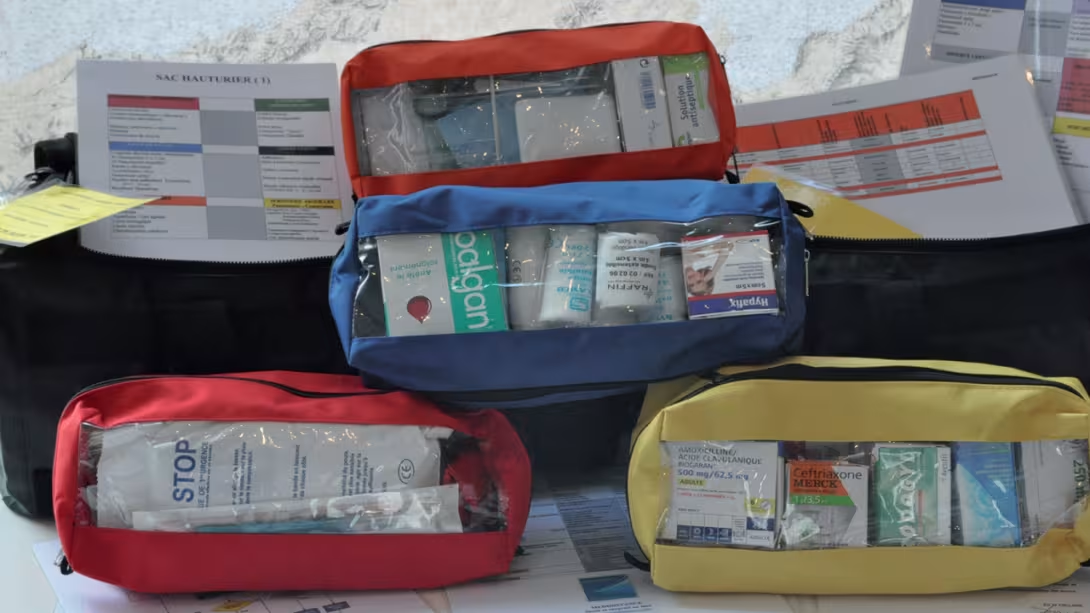
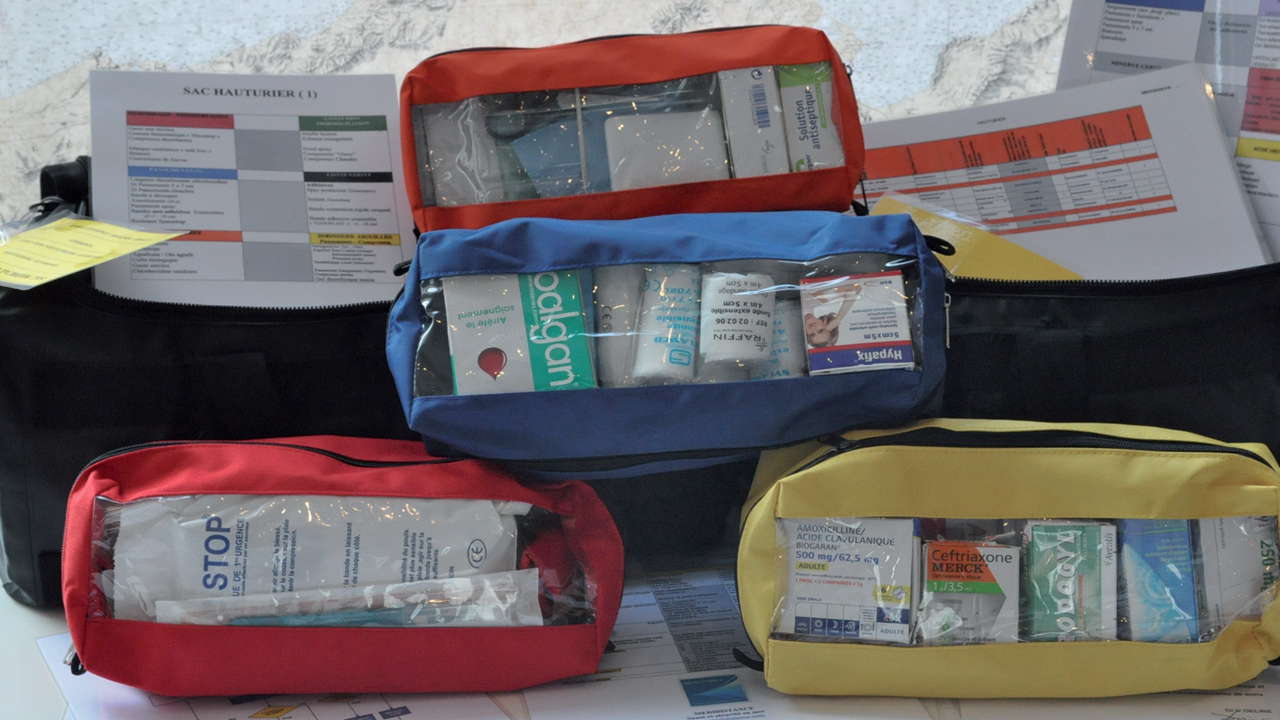
Your local pharmacy is out of reach after the first few miles you cover. It is therefore essential to be able to deal the majority of problems, and to have a good medical kit on board. This first aid kit should contain the necessary equipment and medications for the main health problems likely to arise.
There is no point in storing crates full of different medications collected from all over the place: the result is most often disappointing: many duplicates and certainly missing essential products. The content must therefore be structured and you should scrupulously respect the pre-established lists adapted to the likely degree of remoteness, such as those in France proposed by the Toulouse Medical Consultation Center (CCMM), or similar organizations in your home country.

The CCMM, for example, proposes three types of kit, according to the distance from shore (less than 6 miles, from 6 to 60 miles, more than 60 miles).
It’s obvious that most of the time the use of such equipment and the administration of drugs will be carried out on the advice of the doctor from a distance.
Once on board, this equipment will be stored in an accessible place for when needed, and known to the crew. It needs to be protected from moisture and heat.
With months of happiness passing on the water, you mustn’t forget to maintain your on-board pharmacy in good order, and replace the used or expired drugs. This replenishment can sometimes be complicated. Aboard sailboats, without systematic revisions, a fully stocked medical kit is a rarity.
Personal medication and products needed for travel in hot countries (anti-mosquito, anti-malarial, sun protection...) will of course also be part of the trip.
The skipper will also ensure that the boat is equipped with decent communications equipment. Mobile terrestrial or VHF networks are quickly out of reach and useless at long distances. In order to get in touch with a telemedicine center or the rescue authorities, satellite communications (Iridium, Inmarsat...) need to be available on board.
4- Informing the telemedicine and rescue authorities
Before you cast off towards distant paradise horizons, there’s one last formality: lodging medical details ashore. In France, medical questionnaires can be completed by the members of the crew and returned to the CCMM, along with the list of medicines and the means of communication on board. It is also useful to send the Coastguard an email float plan or traffic report including the boat's contact details and the intended route.
Once you have let slip the lines
On board, prevention is the key to avoiding any "stupid" incidents. Traumas which often occur during maneuvers, or when cooking or fishing can usually be avoided. Preventing the serious man-overboard incident, linked to high mortality, needs to be the subject of your full attention. Respect of the elementary rules of hygiene (food and drinks) are essential to reduce the risk of infectious digestive pathologies.
When a problem arises:
At stopovers, the use of local shore-based care and facilities is the rule. In some countries, the supply of care is deficient (availability, quality, distance). The language barrier can be an added difficulty. The doctor from the health assistance you have subscribed to can be an important logistical aid.

At sea, how to get medical advice or assistance?
When an incident occurs, every sailor should be aware that medical help can be obtained.
The world's oceans are divided up into SAR zones (Search and Rescue). These are attached to the various Maritime Rescue Coordination Centers (MRCC) of maritime nations.
Closely linked to MRCCs, TMAS (Tele-Medical Assistance Service) are structures dedicated to the management of medical problems at sea. In France, this service is provided by the Toulouse Samu regulatory center and its specialized maritime medicine branch: the CCMM. In most countries, initial contact is made with the coastguard who will transfer or relay your communications to the medical authority.
The sailor can be confronted with two situations of different gravity: a medical problem which seems non-urgent, but requires an opinion and therefore a remote consultation; or the situation is immediately worrying and urgent medical intervention is essential.

When a sailor needs medical advice or consultation, he or she directly contacts the Medical Assistance Service (TMAS) or through the Coastguard MRCC. As with most countries, in France, the Center for Maritime Medical Consultations (CCMM) is reachable 365 days a year and 24hours a day. It is advisable to seek their advice for anyone who is ill, injured, intoxicated or who has suffered burns, as well as before any drug administration.
When urgent medical help is required, the sailor should contact the local MRCC. These will trigger the rescue and put the crew in contact with the TMAS or the CCMM.
The decision to carry out the care on board, to divert the boat or to initiate a medical evacuation is decided jointly by the Coastguard MRCC and the medical authorities.

There have been many good examples which demonstrate the effectiveness of this system of medical aid at sea, even in case of significant distances.
Remoteness at sea or the difficulty of access to quality care ashore underline the crucial role of prevention in maintaining the health of those on board.
But if medical care is required, it will be made possible and efficient by means of appropriate communications, prior specific medical training for the crew and having a complete and well thought-out medical kit on board. This preparation will provide for much more serene sailing and stopovers.
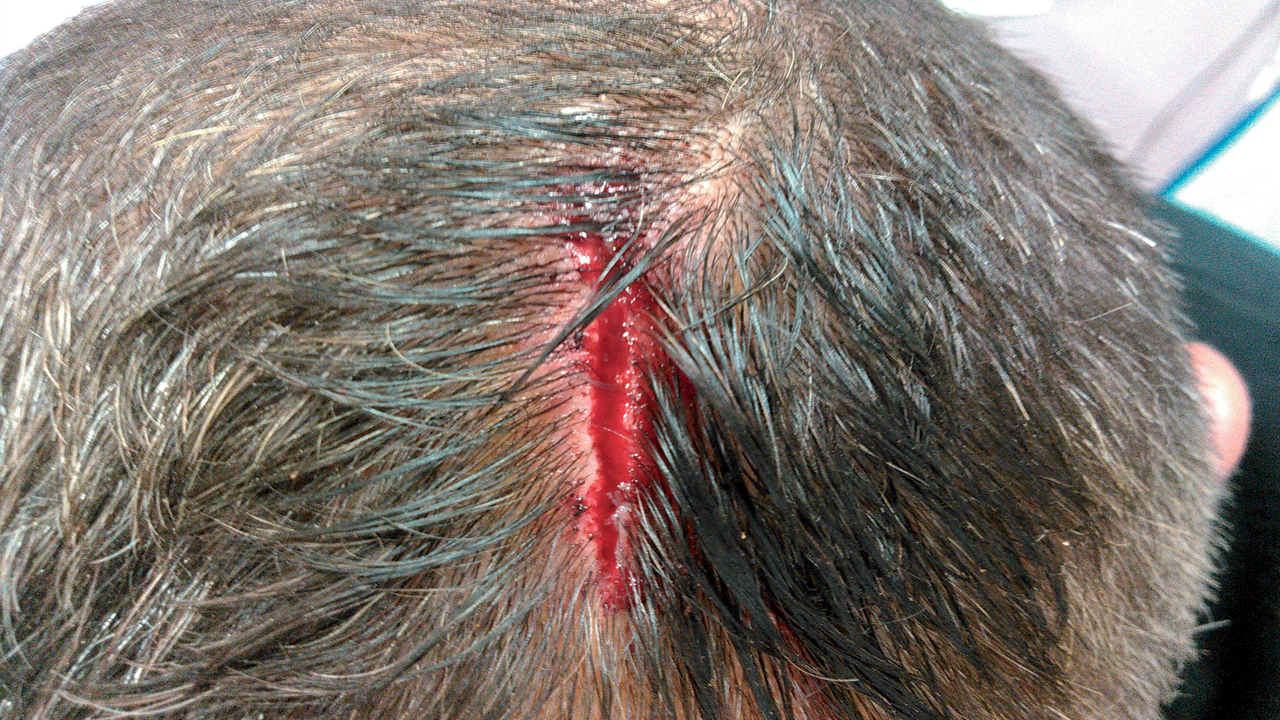
Table 1 – Who were the crews which responded to the Médidistance survey?
|
412 boats sailing in different parts of the world, between 2012 and 2016, for periods of 6 months to more than 2 years, were contacted. More than a quarter of the crews completed the questionnaire listing the medical problems that they were confronted with, at sea or ashore. In addition, to ensure the validity of the overall results of the survey, twenty boats were exhaustively monitored for 10 months around the Atlantic in 2016. Their sailing zones were mainly Atlantic (44%) but some took advantage of the Pacific (19%), the mildness of the Caribbean (13%) or European waters (11%), and one-third of the crews were families with children.
|
Table 2 – Medical problems.
|
Types of problems encountered: 56% illness; 44% injuries. |
|||
|
Frequency: |
½ of the boats (49%)declared at least 1 incident : Average of 2.5 incidents / boat declared. |
51% declared no incidents |
|
|
Place of occurrence : |
At sea:51% |
At sea and ashore: 25% |
Ashore: 24% |
Table 3- INJURIES: 44% of incidents encountered
|
Wounds |
42% |
1/5 linked to fishing |
|
Sprains and fractures |
23% |
Falls or contact with structures |
|
Burns |
15% |
Galley, working or ropes |
|
Origin from marine wildlife |
12% |
Jellyfish; scorpion fish |
|
Head injuries |
1% |
With head trauma, evacuation |
|
Others |
6% |
Tendonitis, dental breakages |
Table 4 – ILLNESSES: 56 % of problems encountered
|
Digestive |
30% |
Severe gastro-enteritis |
|
Urological and/or renal |
16% |
Infections and kidney stones |
|
Ears-Nose-Throat |
15% |
Ear infections and sore throat |
|
Skin |
12% |
Infections |
|
Dental |
8% |
Infections and breakages |
|
Osteo-articular |
6% |
Lumbago and herniated disks |
|
Cardiac and respiratory |
3% |
Infarction, pulmonary infection, asthma |
|
Others |
10% |
Dengue fever, seasickness with dehydration, eye problems and allergies |

Médidistance
Médidistance is a French association which offers medical training in the maritime field. Whether it's organizing the on-board medical equipment, thinking about the vaccines that are essential to the crew depending on the schedule, or preparing to have the right answers in the event of an accident or illness, Médidistance can help you with its team of doctors and sailors... For more information: www.medidistance.com
Other similar organizations exist in most countries, whether private entities or official departments. Advice on where to find training can be obtained from the likes of the RYA in the UK or the SSCA in the USA or others in different countries. For calling for medical help when you are at sea, initial contact can be made with the nearest coastguard, wherever in the world you are.